Narratives of loss: the impact of COVID-19 lockdown on experiences of loss, grief, and bereavement
Rhiannon Dew 1 * , Lis Heath 1 , Richard Egan 2
1 * , Lis Heath 1 , Richard Egan 2
1 Otago Medical School, University of Otago, Dunedin, New Zealand.
2 Department of Preventive and Social Medicine, University of Otago, Dunedin, New Zealand.
Journal of Primary Health Care 14(4) 345-351 https://doi.org/10.1071/HC22090
Published: 17 October 2022
© 2022 The Author(s) (or their employer(s)). Published by CSIRO Publishing on behalf of The Royal New Zealand College of General Practitioners. This is an open access article distributed under the Creative Commons Attribution 4.0 International License (CC BY)
Abstract
Introduction: Restrictions imposed to eliminate the spread of the coronavirus disease 2019 (COVID-19) virus had significant implications on peoples’ experiences of caring for family/whānau at the end of life, and on their own bereavement process.
Aim: This qualitative research explored the impact of COVID-19 lockdown restrictions on experiences of loss, grief and bereavement in Aotearoa New Zealand.
Methods: This qualitative narrative research used semi-structured interviews with 10 participants who experienced the loss of a loved one during Levels 3 or 4 lockdown in Aotearoa New Zealand (23 March–13 May 2020). Interviews were coded using NVivo software and inductive thematic analysis was used to evaluate the data.
Results: Results were grouped into three themes: death experience; mourning in isolation; and availability of support. These themes provide insight into the challenges and difficulties participants faced when they experienced the death of a loved one during a COVID-19 lockdown, and the impact of these restrictions on their experiences of grief and bereavement.
Discussion: The findings from this research suggest there is an increased risk of prolonged grief among those bereaved during lockdown. Primary care professionals need to be aware of this increased risk in order to identify need and provide access to bereavement support.
Keywords: bereavement, COVID-19, grief, prolonged grief disorder.
| WHAT GAP THIS FILLS |
| What is already known: The exceptional restrictions associated with the COVID-19 pandemic have made experiences of death, dying and bereavement uniquely challenging for families/whānau. Research suggests that experiencing the death of a loved one during a COVID-19 lockdown may complicate the grief experience and increase the risk of grief disorders. |
| What this study adds: This small, yet informative study provides insight into the impact COVID-19 lockdown restrictions had on peoples’ experiences of loss, bereavement, and other complex issues surrounding death of a loved one. This research will be useful to primary care professionals when supporting people who experienced a bereavement during a COVID-19 lockdown. |
Introduction
Although the COVID-19 death toll continues to climb around the world, the hidden toll of grief is much higher. Lockdown restrictions in New Zealand meant that individuals and family/whānau who experienced the death of a loved one during this time had to grieve in isolation without the support of friends and whānau who were unable to gather to comfort one another or observe cultural and spiritual rituals associated with grief and mourning. Experience from previous pandemics suggests the impact on cultural norms, rituals and mourning practices around death may affect grief and bereavement outcomes.1 Grief, in and of itself, is an isolating experience, so the requirements for physical distancing, travel restrictions and limits on gatherings are likely to have exacerbated this sense of loneliness and increased the risk for prolonged grief.2
In total, 2509 deaths (including 20 deaths from COVID-19) occurred in New Zealand during the first period of the COVID-19 lockdown (23 March–13 May 2020).3 Researchers have estimated that for every death, approximately nine other people are affected.4 This means the ‘grief toll’ in New Zealand during this period was approximately 22 581. Since then, there have been many more COVID-19-related deaths, and although the restrictions have been eased, many restrictions remain in place and the grief toll keeps rising. It is therefore important to understand the unique needs of those who experienced a bereavement during this time to inform future planning, influence healthcare provider policies and the provision of bereavement support.
On 25 March 2020, the New Zealand Government initiated an Alert Level 4 nationwide lockdown to eliminate the spread of the COVID-19 virus.5 At Alert Level 4, all but essential travel was prohibited, gatherings (including funerals and tangihanga) were cancelled, businesses closed, and people were required to work and learn from home.5 Physical contact was limited to those in the immediate household ‘bubble’, and hospital visiting was strictly prohibited unless on compassionate grounds, in which case, permission had to be granted by the Charge Nurse involved.5 Under Alert Level 3, household ‘bubbles’ could be extended to include close family members or caregivers, and gatherings of up to 10 people for funerals and tangihanga were permitted.5 Under the National Hospital Response Framework in Levels 3 and 4, hospitals were directed to divert people who were dying to alternative providers to ease pressure on hospital beds.6 These restrictions caused major disruptions for families who were unable to be at their loved one’s bedside, say goodbye or observe important cultural or spiritual rituals at the end of life.7 Some families and whānau chose to postpone funerals and tangihanga, whereas others delayed or adapted their mourning processes by using technology to facilitate communication while adhering to restrictions.7,8
Funeral directors play a crucial role in supporting the bereaved by ensuring funerals are personal and meaningful, thus allowing families to achieve a sense of control despite restrictions.9 For a ‘good death’ under COVID-19, every effort should be made to ensure appropriate consultation has been conducted with community members, and that restrictions are seen to be proportionate to the effect of the pandemic.10 An understanding of cultural protocols around death and mourning is paramount, as delaying funerals and tangihanga could have significant implications for cultural, spiritual, and mental health.8,9
For example, for many Māori whānau, tikanga (customary practices or behaviours) suggests whānau care for their loved ones at home wherever possible;11 however, COVID-19 restrictions meant this responsibility could not be shared with the wider whānau and the cultural protocol of whānau staying with the tūpāpaku (deceased) at all times until burial could not be observed. Moeke-Maxwell et al.12 describe the challenges her whānau experienced when arranging a tangihanga during lockdown, including: no internet access at the urupā (burial ground) to enable whānau to watch the ceremony; conducting the entire ceremony on Zoom; and having to decide whether to postpone the tangihanga.
International research suggests stronger grief reactions are evident among family members experiencing a COVID-19 related loss.13 Higher rates of COVID-19-related bereavement yield higher rates of grief disorders, such as prolonged grief and post-traumatic stress disorder.13–15 Prolonged grief disorder (PGD) is defined as persistent and pervasive longing for the deceased and/or cognitive preoccupation with the deceased, combined with intense emotional pain for at least 6 months after bereavement.16 Specific factors associated with the COVID-19 lockdown could bring about longer and more intense grief processes.1 These factors include isolation from family/whānau, social and community support, physical barriers preventing timely communication, and limited opportunities to ‘say goodbye’.1
Many studies have predicted increased rates of prolonged grief, but none (to the best of our knowledge) have confirmed this anticipated affect.16–20 Eisma and Tamminga21 found experiencing a loss during the COVID-19 pandemic elicited more severe grief reactions; however, due to time criteria (6 months post-loss for PGD), they were unable to examine the prevalence of PGD. Goveas and Shear,18 outlined the risk factors for PGD for those bereaved during COVID-19, hypothesising that the circumstances, context and consequences of death during COVID-19 include several risk factors that raise the risk of PGD.18 Comparable risk factors are widely discussed by others, including: unexpected or sudden death of a loved one, difficulties receiving social and emotional support, restricted physical contact, and fewer opportunities to ‘say goodbye’.1,7,18,19,21,22 Uncertainty surrounding COVID-19, travel restrictions, financial hardship, loss of work and disruptions in living arrangements add to potential stressors.1,14,20 Further research is needed to understand the impact of COVID-19 lockdown restrictions on individual and family/whānau experiences of bereavement, and the associated risk of PGD.18,20 Understanding these risk factors is essential for early identification and prevention of harm.21,23
As the world learns to live with the COVID-19 virus, the emergence of new variants reminds us there is no room for complacency. This research provides insight into the lived experience of bereavement during COVID-19 restrictions in a field that is dominated by a biomedical narrative.24
Methods
This qualitative narrative research used semi-structured interviews25 to explore the impact of COVID-19 Levels 3 and 4 lockdown restrictions on peoples’ experiences of loss, grief and bereavement in Aotearoa New Zealand. Critical realism informed this study, allowing for a pragmatic process to understand participants’ experiences;26 that is, critical realism ‘helps researchers to explain social events and suggest practical policy recommendations to address social problems’.26, p. 181 This study design aimed to understand real-world COVID-19 grief experiences to help inform policy and practice.
The study was reviewed and approved by the University of Otago Human Ethics Committee in March 2021 (ref #H21/008). Participants were recruited from the Otago and Southland regions through an article published in local community newspapers and through the researchers’ networks. The researchers hoped the newspaper article would reach participants of diverse age, sex, ethnicity and spiritual backgrounds, while offering distinct experiences of death and bereavement across the Otago and Southland region. Recruitment took place during April and May 2021. Potential participants contacted the researchers via email or phone, and were considered eligible if they had experienced the death of a close friend or family/whānau member during COVID-19 Levels 3 or 4 lockdown in New Zealand (23 March–13 May 2020), the death was not unexpected, they had good spoken English, were aged >18 years, and had access to a computer with reliable internet access. Exclusion criteria included an unexpected cause of death and a previous bereavement(s) within 1 year of their most recent loss, which would have increased the risk of a complicated grief process outside of lockdown restrictions. Thirteen potential participants contacted the primary researcher, out of which 10 were selected who met the inclusion criteria. The information sheet and consent form were emailed to selected participants with a follow-up phone call to answer questions. The interview questions were emailed in advance to enable participants to prepare. Written consent was obtained before proceeding with each interview, which was carried out at a mutually agreed time and place. Due to the emotive subject, participants could have a support person present if they wished. They were also aware of their right to stop the interview or withdraw from the research at any time. A list of support services was provided, with provision for one paid visit to a general practitioner for any participants who wished to access further support. In Aotearoa New Zealand, general practices are private businesses, enrolled patients have their fees subsidised by the Government, with the level of co-payment required determined by the practices. A follow-up phone call 1 week after each interview was also carried out to thank them for their participation and offer support if required.
Data collection
Detailed qualitative data were collected via semi-structured interviews.25 Reflexivity was discussed among the researchers, acknowledging the role and impact of the interviewer and emotive nature of the subject.27 Of the 10 participants, nine interviews were carried out face-to-face, and one took place on Zoom. A combination of open and closed questions were used to explore the impact of COVID-19 lockdown restrictions on participants’ experiences of death and bereavement, including adaptations, coping strategies and the use of bereavement support services.
Data analysis
Interviews were recorded and transcribed using otter.ai. Participants shared deeply personal and emotive stories during the interviews; for this reason, transcripts were returned to each participant to check for accuracy and allow for further comment. No changes or edits were made. Transcripts were coded using NVivo software (QSR International). Inductive thematic analysis25 was conducted by the researcher (RD) to derive themes from the raw data. Codes were manually applied throughout the data and initial themes developed from the codes. One transcript was selected and coded independently by all authors to compare for consistency and coding styles. Initial themes were then consolidated into three main themes through critical dialogue with all authors. Pseudonyms were used to protect anonymity and ensure confidentiality.
Results
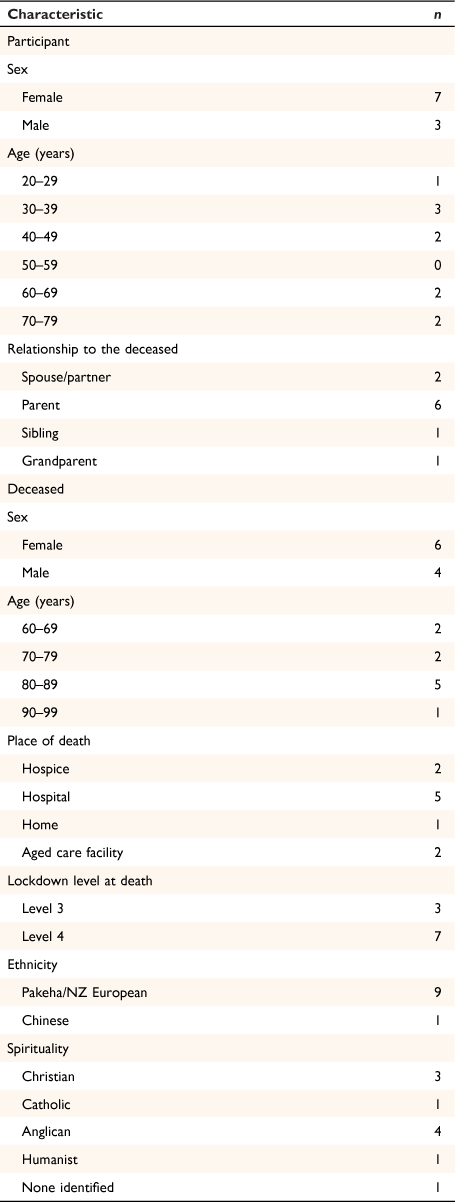
Of the 10 participants, seven were female and three were male. Relationships to the deceased included spouse/partner (n = 2), parent (n = 6), sibling (n = 1) and grandparent (n = 1). Participant characteristics are provided in Table 1. Three major themes were identified: (1) death experience; (2) mourning in isolation; and (3) availability of support. Of the 10 participants, five experienced the death of their family member in a hospital setting, and two required hospital-level care in the days before death.
|
Theme 1: death experience
Experiencing the death of a loved one during a COVID-19 lockdown brought about unique and distressing experiences. Travel and hospital visitation restrictions meant many family members were unable to be with their loved one at the end of life, denying them the opportunity to ‘say goodbye’ and have important conversations. These restrictions had a profound impact on participants’ death experiences; for example:
I wanted to be with her, have her in my arms and holding her hands reassuring her and telling her, I’d be there for her…. I couldn’t do any of it because I wasn’t allowed in the room. (Audrey)
Visiting restrictions also forced families to choose one family member to stay with their loved one until they died. No additional support person to relieve the one nominated person was allowed.
My brother came half an hour later on; they didn’t let him in at all. Which I didn’t know about because I was already in there. For him, it was hard, because he never saw her the day she died but I did. (Alison)
Participants struggled with the ever-changing rules enforced by health authorities, which compounded families’ stress by requiring them to constantly adapt; for example:
I think one of the things about it was that no one really knew the rules. (Luke)
The way in which the visiting rules were enforced by hospital staff also caused significant confusion and distress; for example:
My family members were saying one day we were at this door, and then the next day a nurse would yell at us and tell us to go the other door, you weren’t meant to be at that door and then they’d say you’ve got to go through the hospital, not on the outside of the hospital, and it was just nuts. (Nancy)
Others commented that it appeared the healthcare system’s sole focus was on COVID-19 as hospital staff and resources prepared for an influx of COVID-19 patients, rather than supporting those who were dying, for example: “I found it very difficult at first because the hospital was so focused on getting ready for this huge event and Chris was dying. I had to really push, sometimes for him to get the pain relief he needed.” (Anne)
Participants observed a variety of responses from healthcare workers. Some were empathetic and helped ‘bend’ the rules for compassionate reasons, whereas others carefully obeyed the rules and enforced the strict visitation polices; for example:
When they got down to the ambulance, the worst thing about it was I knew all the rules about the fact that we weren’t allowed to take family members to ED. So I thought things were going bad. However, the senior ambo on the crew, the senior paramedic said “look we’ll just break the rules, we’ll take your mother with us.” So my mother hopped in the front of the ambulance and off they toddled to ED. (Luke)
Participants’ responses to strictly enforced restrictions also varied; for example:
I went into hospice and they wouldn’t let me visit. I could go in I could stay in, and so I did. And they locked us in a room, and we weren’t allowed even out into the passage. Yeah, it’s pretty dreadful. (Lennon)
Although these restrictions were a necessary part of the COVID-19 response, they caused a great deal of distress for participants and their family/whānau at an emotionally difficult time. The speed and unprecedented context in which these restrictions were imposed meant participants had no time to prepare and found their ‘last goodbyes’ play out in a way they could not have anticipated.
Theme 2: mourning in isolation
Of the 10 participants, seven experienced the death of their loved one during Level 4 lockdown, with the remaining three in Level 3 lockdown, in the days immediately preceding the transition to Level 4 lockdown. Consequently, all 10 participants were acutely grieving during Level 4 lockdown. Isolation, loneliness, and fear characterised participants’ experiences during this time.
Appalling. It couldn’t have been worse. It just dragged the whole thing out and made it, and the isolation factor was just absolutely beyond belief. (Lennon)
Common rituals and practices around death and mourning were suspended during Level 4 lockdown, so friends and families could not gather to support one-another in their grief. For some, this meant that memorial services were delayed until they could be conducted in person when restrictions were lifted. Others chose to proceed despite many being unable to attend.
We have the ceremonies of funeral and mourning for a reason because they help you mourn; they can release things and I mean that was…we did get that but it was a really dragged-out process…. The restrictions became a bit looser, there were options to have 10 people at a funeral service/memorial service, and that’s not okay. Well, it wasn’t okay for us because what do you do? There are more than 10 people in our family, yeah. And then you could have gatherings of 100, and it was like, so the 100 and 10th person comes and you turn them away? Which 100 people are more important? You can’t do that. So, we waited. We waited until the restrictions were over. (Olive)
Participants commented on the desire to grieve and be consoled by warmth, touch and embrace; however, the requirement for social distancing removed the human connection. So, not only did the death experience change, it resulted in a sense of profound loneliness; for example:
Imagine having a funeral without being able to hug each other? Just to be that close to the person you love and want to support, it was shit being away from each other, but at least you weren’t tortured by the ‘you’re there but I still can’t hug you’. That would have been appalling to me. (Olive)
Theme 3: availability of support
Participants commented on the difficulty accessing support while caring for their loved one at home; for example:
We have these little rituals that are part of the process. And when they don’t occur as they should occur, it upsets you because they are so useful. We get together, we look after one another and so when you can’t do that… (Lennon)
Of the 10 participants, only two accessed formal bereavement support. Both remarking how useful it was.
The counselling, wherever it came from, I really valued it, and I would hope that would always be available to people regardless. (Anne)
Lockdown restrictions also impacted support networks, from a noticeable lack of cards and meals prepared by friends and community members, to the difficulty accessing support from hospice and other healthcare providers. The loss of these simple, yet important gestures and support services compounded participants’ sense of isolation.
Discussion
The unprecedented nature and speed with which New Zealand entered Levels 3 and 4 lockdown in March 2020 meant there was a lack of guidelines at the time as to how to meet the needs of family/whānau when caring for people at the end of life under lockdown conditions. The New Zealand government’s ‘Unite against COVID-19’ campaign helped develop a collective sense of purpose among New Zealanders, with opinion polls showing >80% support for the government’s actions.28,29 Although it may have been understood that these restrictions were put in place to protect the wider community, the impact of lockdown on peoples’ experiences of death and dying had significant implications on their grief and bereavement processes.
Recent literature notes specific factors associated with the COVID-19 pandemic have brought about profound challenges for those bereaved, including limited contact with their dying loved one, social isolation, and loneliness.1,10,30,31 This study provides insight into similar issues participants faced when grieving during lockdown in Aotearoa New Zealand. Although these findings are not generalisable to the whole population, they illuminate issues that people in similar situations may experience. Certain aspects of their experience compounded their grief and hindered the bereavement process, increasing the risk of prolonged grief. These factors included having to adjust to rules that were constantly changing, which created confusion and distress; the loss of family and community support; and difficulty accessing support services, especially for those who had been caring for a loved one at home.
The risk for prolonged grief following a COVID-19-related death has been discussed widely,18,20–22,32,33 specific circumstances, context and consequences surrounding the COVID-19 pandemic likely elevating the risk for PGD.18 Eisma et al.32 notes specific learning from COVID-19’s impact on bereavement is pertinent, as it is thought the risk for severe and prolonged grief will become a worldwide public health concern. Since this research was conducted, Aotearoa New Zealand has seen the emergence of the Delta, Omicron and subsequent variants with widespread community transmission. This highlights the fact that although we may no longer be in lockdown, the risk for prolonged grief persists for those who experienced a bereavement during that time, with an ever-present threat of a return to COVID-19 restrictions in the future.
Similar studies have been published sharing experiences of those bereaved during the COVID-19 pandemic.15,22,31,34,35 These studies stress the importance of open communication from healthcare providers, allowing the opportunity to ‘say goodbye’, and provision of bereavement support. This study is the first step towards understanding the impact that COVID-19 restrictions had on experiences of loss, grief and bereavement in Aotearoa New Zealand, in an effort to raise awareness of the needs of those bereaved during this time, so the necessary supports can be provided. Potential support includes increased funding for bereavement support services to ensure they are available, accessible and promoted within all communities. Clear and compassionate communication between healthcare providers and family/whānau when caring for people at the end of life under changing COVID-19 restrictions is also important to avoid confusion and further distress. That is, based on our findings, this includes sensitively communicating changing rules and restrictions and facilitating opportunities for family/whānau to ‘say goodbye’.
Although our small sample was informative, extending this study to include a larger number of participants from a variety of cultural groups, faith traditions and geographic locations would provide greater understanding of the issues involved and the support structures required. This study did not include relatives' experiences when a deceased death was unexpected, nor did it identify any differences in bereavement outcomes due to cause or place of death. Selman et al.22 notes COVID-19 deaths, unexpected deaths, hospital and care home deaths were associated with poorer end-of-life care and COVID-19 pandemic-related challenges in bereavement. Future research could focus on family/whānau experiences of COVID-19-related deaths, Residential Age Care Facility responses to COVID-19, and healthcare professionals’ perspectives of caring for patients and family/whānau during the COVID-19 pandemic. The findings from this study provide insight into the lived experiences of those bereaved during lockdown in Aotearoa New Zealand. This research highlights the profound impact that COVID-19 restrictions had on the bereaved, the increased risk for prolonged grief among this group of people, and the need for bereavement support to be an essential part of healthcare policy and provision.
Data availability
The data that support this study cannot be publicly shared due to ethical or privacy reasons and may be shared upon reasonable request to the corresponding author, if appropriate.
Conflicts of interest
The authors declare no conflicts of interest.
Declaration of funding
We are grateful to the Otago Medical School Dean’s Research Scholarship that facilitated RD’s capacity to do this research.
References
[1] Mayland CR, Harding AJE, Preston N, et al. Supporting adults bereaved through COVID-19: a rapid review of the impact of previous pandemics on grief and bereavement. J Pain Symptom Manage 2020; 60 e33–9.| Supporting adults bereaved through COVID-19: a rapid review of the impact of previous pandemics on grief and bereavement.Crossref | GoogleScholarGoogle Scholar |
[2] Frangou C. The pandemic has disrupted death and mourning in ways we don’t yet understand. Canada: St. Joseph Communications; 2020. Available at https://www.macleans.ca/society/covid-19-pandemic-disrupted-death-mourning-grief/ [Updated 15 July 2020; Accessed 2 August 2020].
[3] StatsNZ. COVID-19 data portal. Wellington, New Zealand: New Zealand Government; 2021. Available at https://www.stats.govt.nz/experimental/covid-19-data-portal?tab=Health&category=Weekly%20deaths [Accessed 6 April 2021].
[4] Verdery AM, Smith-Greenaway E, Margolis R, et al. Tracking the reach of COVID-19 kin loss with a bereavement multiplier applied to the United States. Proc Natl Acad Sci 2020; 117 17695–701.
| Tracking the reach of COVID-19 kin loss with a bereavement multiplier applied to the United States.Crossref | GoogleScholarGoogle Scholar |
[5] Government NZ. New Zealand Covid-19 Alert Levels. 2020. Available at https://covid19.govt.nz/assets/resources/tables/COVID-19-alert-levels-detailed.pdf [Accessed 26 January 2021].
[6] Ministry of Health. COVID 19 National Hospital Response Framework – The Process. Wellington: Ministry of Health; 2020. Available at https://www.adhb.health.nz/assets/Documents/OIA/2021/09-21/OIA-964-3.-National-Hospital-Response-Framework-V2-210420.pdf [Accessed 17 November 2021].
[7] Wallace CL, Wladkowski SP, Gibson A, et al. Grief during the COVID-19 pandemic: considerations for palliative care providers. J Pain Symptom Manage 2020; 60 e70–6.
| Grief during the COVID-19 pandemic: considerations for palliative care providers.Crossref | GoogleScholarGoogle Scholar |
[8] Mclachlan L-M. COVID-19 funeral restrictions leave families grieving in isolation. New Zealand: Radio New Zealand; 2020. Available at https://www.rnz.co.nz/news/te-manu-korihi/412705/covid-19-funeral-restrictions-leave-families-grieving-in-isolation [Updated 26 March 2020; Accessed 22 July 2020].
[9] Burrell A, Selman LE. How do funeral practices impact bereaved relatives’ mental health, grief and bereavement? A mixed methods review with implications for COVID-19. OMEGA J Death Dying 2020; 85 345–83.
| How do funeral practices impact bereaved relatives’ mental health, grief and bereavement? A mixed methods review with implications for COVID-19.Crossref | GoogleScholarGoogle Scholar |
[10] Bear L, Simpson N, Angland M, et al. ‘A good death’ during the Covid-19 pandemic in the UK: A report on key findings and recommendations. 2020. Available at http://eprints.lse.ac.uk/104143/
[11] Oetzel J, Simpson M, Berryman K, et al. Managing communication tensions and challenges during the end-of-life journey: perspectives of Māori kaumātua and their whānau. Health Commun 2015; 30 350–60.
| Managing communication tensions and challenges during the end-of-life journey: perspectives of Māori kaumātua and their whānau.Crossref | GoogleScholarGoogle Scholar |
[12] Moeke-Maxwell T, Nikora LW, Mason K, et al. Te Whakatara! – Tangihanga and bereavement COVID-19. Ethnographic Edge 2020; 4 19–34.
| Te Whakatara! – Tangihanga and bereavement COVID-19.Crossref | GoogleScholarGoogle Scholar |
[13] Borghi L, Menichetti J, Vegni E, et al. A phone-based early psychological intervention for supporting bereaved families in the time of COVID-19. Front Public Health 2021; 9 625691
| A phone-based early psychological intervention for supporting bereaved families in the time of COVID-19.Crossref | GoogleScholarGoogle Scholar |
[14] Morris SE, Moment A, Thomas Jd. Caring for bereaved family members during the COVID-19 pandemic: before and after the death of a patient. J Pain Symptom Manage 2020; 60 e70–4.
| Caring for bereaved family members during the COVID-19 pandemic: before and after the death of a patient.Crossref | GoogleScholarGoogle Scholar |
[15] Donnelly S, McDonald F, Goodyer C. Whānau experiences of patients’ deaths in Wellington Hospital during 2020 COVID-19 pandemic Levels 3 & 4. N Z Med J 2022; 135 16
[16] Eisma MC, Boelen PA, Lenferink LIM. Prolonged grief disorder following the Coronavirus (COVID-19) pandemic. Psychiatry Res 2020; 288 113031
| Prolonged grief disorder following the Coronavirus (COVID-19) pandemic.Crossref | GoogleScholarGoogle Scholar |
[17] Carr D, Boerner K, Moorman S. Bereavement in the time of coronavirus: unprecedented challenges demand novel interventions. J Aging Soc Policy 2020; 32 425–31.
| Bereavement in the time of coronavirus: unprecedented challenges demand novel interventions.Crossref | GoogleScholarGoogle Scholar |
[18] Goveas JS, Shear MK. Grief and the COVID-19 pandemic in older adults. Am J Geriatr Psychiatry 2020; 28 1119–25.
| Grief and the COVID-19 pandemic in older adults.Crossref | GoogleScholarGoogle Scholar |
[19] Mortazavi SS, Assari S, Alimohamadi A, et al. Fear, loss, social isolation, and incomplete grief due to COVID-19: a recipe for a psychiatric pandemic. Basic Clin Neurosci 2020; 11 225–32.
| Fear, loss, social isolation, and incomplete grief due to COVID-19: a recipe for a psychiatric pandemic.Crossref | GoogleScholarGoogle Scholar |
[20] Stroebe M, Schut H. Bereavement in times of COVID-19: a review and theoretical framework. OMEGA J Death Dying 2021; 82 500–22.
| Bereavement in times of COVID-19: a review and theoretical framework.Crossref | GoogleScholarGoogle Scholar |
[21] Eisma MC, Tamminga A. Grief before and during the COVID-19 pandemic: multiple group comparisons. J Pain Symptom Manage 2020; 60 e1–4.
| Grief before and during the COVID-19 pandemic: multiple group comparisons.Crossref | GoogleScholarGoogle Scholar |
[22] Selman LE, Farnell D, Longo M, et al. Risk factors associated with poorer experiences of end-of-life care and challenges in early bereavement: results of a national online survey of people bereaved during the COVID-19 pandemic. Palliat Med 2022; 36 717–29.
| Risk factors associated with poorer experiences of end-of-life care and challenges in early bereavement: results of a national online survey of people bereaved during the COVID-19 pandemic.Crossref | GoogleScholarGoogle Scholar |
[23] Selman LE, Chao D, Sowden R, et al. Bereavement support on the frontline of COVID-19: recommendations for hospital clinicians. J Pain Symptom Manage 2020; 60 e81–6.
| Bereavement support on the frontline of COVID-19: recommendations for hospital clinicians.Crossref | GoogleScholarGoogle Scholar |
[24] Moeke-Maxwell T, Collier A, Wiles J, et al. Bereaved families’ perspectives of end-of-life care. Towards a bicultural Whare Tapa Wha older person’s palliative care model. J Cross Cult Gerontol 2020; 35 177–93.
| Bereaved families’ perspectives of end-of-life care. Towards a bicultural Whare Tapa Wha older person’s palliative care model.Crossref | GoogleScholarGoogle Scholar |
[25] Patton MQ. Qualitative research and evaluation methods, 3rd edn. Thousand Oaks: Sage; 2002.
[26] Fletcher AJ. Applying critical realism in qualitative research: methodology meets method. Int J Soc Res Methodol 2017; 20 181–94.
| Applying critical realism in qualitative research: methodology meets method.Crossref | GoogleScholarGoogle Scholar |
[27] Underwood M, Satterthwait LD, Bartlett HP. Reflexivity and minimization of the impact of age-cohort differences between researcher and research participants. Qual Health Res 2010; 20 1585–95.
| Reflexivity and minimization of the impact of age-cohort differences between researcher and research participants.Crossref | GoogleScholarGoogle Scholar |
[28] Jamieson T. “Go hard, go early”: preliminary lessons from New Zealand’s response to COVID-19. Am Rev Public Adm 2020; 50 598–605.
| “Go hard, go early”: preliminary lessons from New Zealand’s response to COVID-19.Crossref | GoogleScholarGoogle Scholar |
[29] Cooke H. Coronavirus: public surge in trust of Government during Covid-19 crisis. Stuff, 8 April 2020. Available at https://www.stuff.co.nz/national/health/coronavirus/120911320/coronaviruspublic-surge-in-trust-of-government-and-national-pride2022 [Accessed 2 September 2022]
[30] Selman L. Covid grief has cracked us open: how clinicians respond could reshape attitudes to bereavement—an essay by Lucy Selman. BMJ 2021; 374 n1803
| Covid grief has cracked us open: how clinicians respond could reshape attitudes to bereavement—an essay by Lucy Selman.Crossref | GoogleScholarGoogle Scholar |
[31] Hanna JR, Rapa E, Dalton LJ, et al. A qualitative study of bereaved relatives’ end of life experiences during the COVID-19 pandemic. Palliat Med 2021; 35 843–51.
| A qualitative study of bereaved relatives’ end of life experiences during the COVID-19 pandemic.Crossref | GoogleScholarGoogle Scholar |
[32] Eisma MC, Tamminga A, Smid GE, et al. Acute grief after deaths due to COVID-19, natural causes and unnatural causes: an empirical comparison. J Affect Disord 2021; 278 54–6.
| Acute grief after deaths due to COVID-19, natural causes and unnatural causes: an empirical comparison.Crossref | GoogleScholarGoogle Scholar |
[33] Varshney P, Prasad G, Chandra PS, et al. Grief in the COVID-19 times: are we looking at complicated grief in the future? Indian J Psychol Med 2021; 43 70–3.
| Grief in the COVID-19 times: are we looking at complicated grief in the future?Crossref | GoogleScholarGoogle Scholar |
[34] Harrop E, Goss S, Farnell D, et al. Support needs and barriers to accessing support: baseline results of a mixed-methods national survey of people bereaved during the COVID-19 pandemic. Palliat Med 2021; 35 1985–97.
| Support needs and barriers to accessing support: baseline results of a mixed-methods national survey of people bereaved during the COVID-19 pandemic.Crossref | GoogleScholarGoogle Scholar |
[35] Hamid W, Jahangir MS. Dying, death and mourning amid COVID-19 pandemic in Kashmir: a qualitative study. OMEGA J Death Dying 2020; 85 690–715.
| Dying, death and mourning amid COVID-19 pandemic in Kashmir: a qualitative study.Crossref | GoogleScholarGoogle Scholar |


